Self-care: The 99% of healthcare we ignore
Why is self-care important in the context of global health, why we have we ignored it for so long, and how AI is opening up another window for a long-overdue revolution
Thanks to everyone who commented, replied by email and posed related questions to explore in response to my last post on AI singularities — it seemed to strike a raw nerve, and your reflections gave me a lot of food for thought that I will hopefully dive more into in this and future posts. Please keep them coming.
***
What is self-care and how important is it?
If you are anything like me, you probably spend a LOT more time in health-related self-care than you spend under professional/clinical healthcare. I don’t mean self-care in the capitalistic way the Western world has reinvented it, conjuring images of expensive detox spas and hot yoga retreats. I mean the banal, everyday things we each do to take care of our own health, starting from brushing our teeth, exercising, having nutritious food, meditating/praying, or maintaining good hygiene and sleep schedules, all the way to managing our pain with an OTC medicine, wearing a condom to prevent STDs, self-testing at home for pregnancy or COVID, or monitoring our diabetes and blood pressure to manage chronic diseases. Here’s a rather comprehensive facts and definitions page from WHO.
A rough back of the envelop calculation yields ~15 hours each week I spend in such activities. Compared with the ~5 doctor and lab visits I have to do each year, in terms of sheer time spent the ratio is at least 150:1! I can also confidently attest that my physical and mental health status is at least 90%+ a result of my daily choices and actions, and <10% attributable to competent clinical care (doctor visits, prescription medicines, therapy, etc.) for the few things I cannot do on my own.

Of course this is also dependent on genetics, age and other risk factors. As a relatively healthy 40-year old living a stable life, my need for clinical care is much lower than anyone with an assortment of inherited illnesses, a displaced refugee, or my healthy 73-year old dad. If you hold these exogenous factors constant (since we cannot influence them easily), I would further posit that the earlier you start on disciplined self-care, the later and lesser in aggregate you will need clinical care. Or more formally:
The most eye-popping example of this I found relates to the emerging evidence around Type-II diabetes reversal. In a randomized trial in Qatar, the treatment group receiving an intensive lifestyle adjustment intervention showed complete remission of diabetes in 61% of cases, and normal blood glucose levels in 33%. Compared to the control group which just received evidence-based clinical care, the lifestyle modification group was 12X (OR=12, 95% CI 5.17-28.03) more likely to be free from any symptoms of diabetes.
This means that not only is self-care powerful in preventing disease, it can even reverse chronic diseases that have long been assumed by the clinical establishment to be lifelong and irreversible. Contrast this with the estimate that diabetics on average lose 13+ years of life from the point of diagnosis, and imagine the potential gains in terms of reducing human suffering and cost burden on the health system from just one lifestyle intervention!
A conceptual model
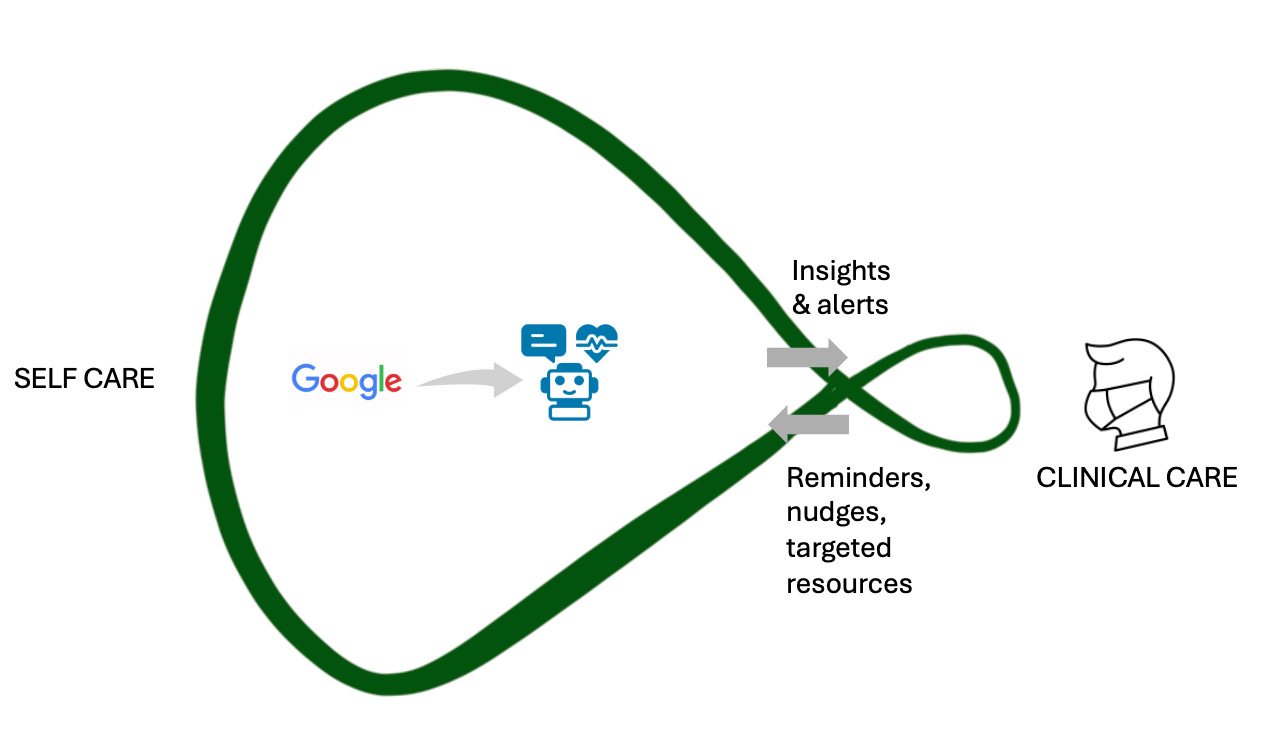
If we follow this train of thinking to its logical endpoint, the ideal design of a health system should be one in which self-care and clinical interventions are part of an integrated care continuum that starts at birth and ends only in death:
In this conceptual model, each time you leave a doctor’s chamber or CHW visit, it informs and hones your self-care routines and practices, which keeps you in good health until the next scheduled encounter or acute incident prompts a touchpoint with the formal health system. Simplistically, your goal is to maximize the self-care loop and minimize the clinical care loop as much as possible.
Indeed, this is kind of what it looks like from the typical patient’s perspective already.
Why are health systems designed so differently then?
It is, at least on the surface, rather mind-boggling how rarely health systems across the world are designed factoring in this essential and primary role of self-care. It does, however, make more sense when you visualize the care continuum as it currently seems from the perspective of a clinician or the health system:
In Bangladesh, I would often hear public sector doctors refer to poor people’s “self-medication” at the pharmacy or their belief in traditional medicines in a derogatory sense, implicitly implying that they are acting against their best interests when it comes to health. I myself have been admonished with “Don’t trust Dr. Google”, and “Don’t come to me if you believe in snake oil” when I went to renowned allopathic doctors after doing my research and trying out alternative therapies.
There are at least a few underlying factors that drive this lack of understanding and appreciation of self-care within our health systems:
Clinical bias: To a hammer, everything looks like a nail. Trained doctors, who tend to drive public health policy as well, are conditioned to think in terms of diagnosing and treating problems, and certainly not from the patients’ perspective, who would rather avoid going to the doctor at all in the first place.
Lack of visibility: We don’t understand what we cannot see. The moment a patient exits the chamber, they become invisible to the “system”, and what they do at home and in their communities are a complete black box.
Lack of actionability and personalization: Even if you knew what people are doing, there are few tools, and even fewer resources, to targetedly intervene in each unique case. So why bother? Might as well focus on blunt tools like behavior change campaigns and hope some of it sticks!
Financing for “sick-care” over true healthcare: Our legacy systems monetize sickness and finance “interventions”, and are not designed to reward keeping people in good health. Hence, preventive mechanisms like self-care are not financed or prioritized.
Prejudices and lack of real empathy for the poor: Last but not least, I have often felt that there is also an implicit bias and prejudice that prevents many clinicians and health systems folks (who tend to represent the upper echelons of society) from truly empathizing with the poor and thinking of their health in the same way we think of our own health needs and aspirations. I fall victim to this bias myself and often have to remind myself of my own needs and experience as a patient and care-seeker.
Given how little we understand and appreciate how people approach and take care of their own health, it should come as no surprise that we struggle to deliver outcomes on anything that requires more than a one-off intervention, and a semblance of a partnership with the individual, their families and their community — antibiotic resistance, tuberculosis, malaria, dengue fever, NCDs like diabetes and hypertension, and mental health are all glaring examples.
If delivering health outcomes is our core objective in designing our health systems, [assuming we can’t greatly influence people’s socio-econo-environmental constraints (a.k.a. social determinants of care)] then we must act as partners in helping them manage their own health better (the 99%) before bringing in the clinical “hammer” for the remaining 1%.
The promise of digitization and AI
Perhaps needless to re-emphasize, but people all over the world, including the poorest, do their best to take care of their own health and well-being given the much larger set of constraints they operate within, which are largely determined by their socio-economic and physical environments, and often also includes poor information.
Digitization has already helped alleviate the information and visibility bottlenecks significantly, even though we have barely taken notice on the public health side of things. In fact, 7% of all google searches (1 billion queries per day) are health related. In India, Prime Minister Modi on an election year was only 2.5x more popular than “diabetes” as a search topic, was at par with “exercise”, and was less than half as popular as “skin” related queries.
Google clearly already has the largest database of self-care queries, and by proxy, interest, anywhere in the world. Combine that with Google Fit (or similar platforms), which is an activity tracker pre-loaded on most of the 3 Billion Android phones in the world, and we also have the world’s largest database of self-care behaviors and activities (daily steps, sleep times, BMI, etc.), even among less well-off populations.
Although there are a plethora of apps for this in the private sector, from a health systems perspective, we have not yet leveraged this newfound visibility to design better self-care oriented interventions or inclusive care continuums. But the size and scope of this opportunity will be amplified another 100x with the advent of clinically competent AI personal health companions.
For example, many of those 1 billion search queries a day are going to become actual clinical consultations, informed by each person’s health history and records, and often done over voice in the user’s natural language. If we design these well, we will gain highly nuanced insights from these conversations about the actions people are taking, and the impact that is having, on their health and well-being. But more importantly, each of those conversations will also be an opportunity for us to inform them with the latest clinically validated information adjusted to their prevailing level of health literacy and understanding (ask ChatGPT to explain Quantum Mechanics for a 6, 12 and 18 year old, to see what I mean), and to influence and nudge their behavior in a highly personalized and contextually appropriate manner. In this new reality, the role of the health system will be to plug into these conversations for insights into people’s health, and to provide targeted resources and interventions to remove bottlenecks. You’re too poor to afford quality food? Let’s connect you to the government rations program. You are struggling to manage your diabetes through nutrition and exercise? Let’s assign a CHW to visit you routinely and supply you your Metformin.
It is important to highlight how significant the personalization aspect of this is. Traditional behavior change campaigns often fail to have significant impact because each individual’s context, preferences and challenges are completely unique. AI can solve the personalization problem once and for all. For example, if I am a poor pregnant woman in rural India and show signs of iron deficiency, it might advise me to grow some spinach on my backyard and increase my lentil consumption:
Just this week, OpenAI and Arianna Huffington’s Thrive Global embarked on a high-profile joint venture to build exactly such an AI “Personal Health Coach” that will remember everything about an individual and provide hyper-personalized and contextually aware nudges to improve one’s preventive behaviors such as exercise, nutrition and sleep. This is only the beginning.
I discussed this impending amplification of the agency and autonomy of individuals, and the role of the health system in this new reality, in more detail under Singularity #3 of my AI post.
A call for re-imagination
Of course building trust in AI health coaches and figuring out their safety guardrails will take some time, and the equity issues are important to think through. We also already spoke about the other systemic barriers we have to overcome, which are non-trivial. Below is a list of the main barriers and potential enablers to help overcome them.
But the first and inevitable step is one of intent and imagination. If we truly believe in building people-centered health systems and want to keep people in good health rather than only treat sickness, we have to prioritize and position self-care as a core, if not the main, engine of healthcare. As a by-product, we might be surprised to stumble upon the most cost-effective way to achieve health outcomes, and a healthy, happy population.
Reorienting ourselves from a top-down, clinically-oriented and system-centered approach towards one that maximizes people’s agency and autonomy to take care of their own health, is LONG overdue. AI might just provide us the best opportunity we have ever had to make that vision a reality, but it is in the end up to us to design and build that future.










